Poikiloderma of Civatte is a chronic sun-related skin change that causes a mottled mix of redness, brown pigmentation and visible small blood vessels on the sides of the neck and sometimes the lower cheeks. It is harmless, but it can be surprisingly difficult to treat. In this article, we’ll explore what causes Poikiloderma of Civatte and best treatments to help get rid of it.
What is Poikiloderma of Civatte?
Although it’s incidence is not known, Poikiloderma of Civatte is thought to be a common benign skin condition that mainly affects sun exposed areas of the face. The most common location is on the sides of the neck and lateral cheeks. It is a combination of skin thinning, pigment change and telangiectasia, which are fine visible blood vessels. In practice, this creates a net-like or patchy appearance with red-brown discolouration on a background of hyperpigmented spots or patches from sun damage.
It’s important to stress that Poikiloderma of Civatte is not dangerous and i mainly a cosmetic concern. However, despite being benign, it is still a marker of chronic sun damage. As such, sun protection is vital not just to reduce progression but also to reduce wider UV-related skin damage and cancer over time.
How Does Poikiloderma of Civatte Look?
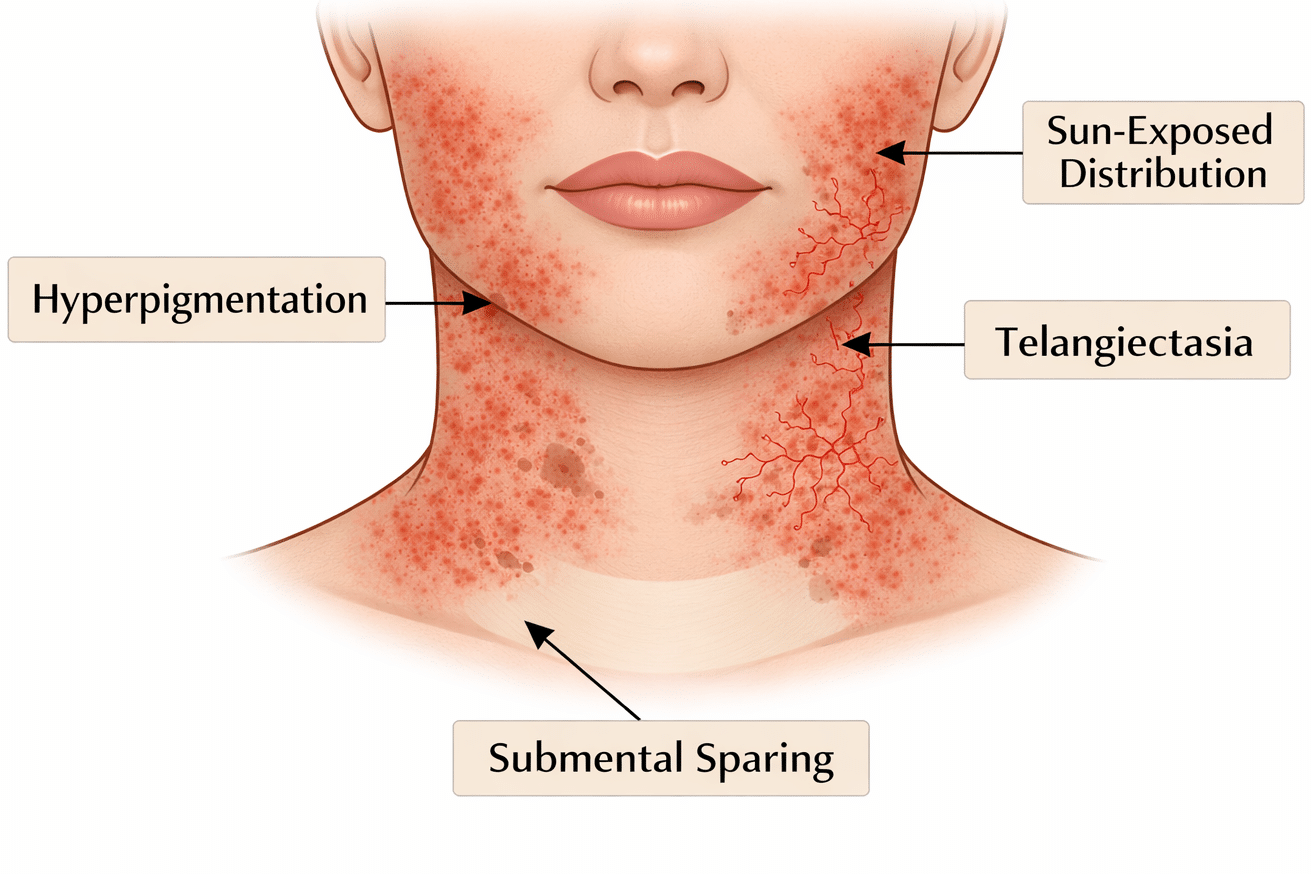
Patients usually notice a persistent patchy or lacy looking discolouration on the sides of the neck and cheeks that gradually becomes more obvious over time. It typically has several features so diagnosis involves looking for:
- Redness: This comes from dilated superficial blood vessels and often gives the neck a flushed or weathered appearance.
- Brown hyperpigmentation: There is often background hyperpigmentation from chronic photodamage, which can make the condition resemble melasma or general sun spots at first glance.
- Fine visible vessels: Small thread veins or telangiectasia are a key part of the diagnosis and help explain why pigment fading creams alone rarely fully clear it.
- Symmetry: It usually affects both sides of the neck in a broadly symmetrical pattern.
- Relative sparing under the chin: The skin in the shaded submental area is often unaffected.
What Causes Poikiloderma of Civatte?
There is not one single cause for Poikiloderma of Civatte. In most patients, it develops through a mix of cumulative ultraviolet exposure, skin ageing and individual susceptibility. It is reported more often in middle-aged and older adults, particularly women. Some research also suggests that photosensitising fragrance or cosmetic ingredients in leave-on products might aggravate the condition in susceptible people. Below are the most common causes for developing Poikiloderma of Civatte:
- Chronic sun exposure: This is thought to be the main driver and explains the typical distribution on exposed areas of the neck and cheeks.
- Photoageing: Long-term UV damage alters pigment handling, damages supporting skin structures and contributes to visible blood vessels and skin thinning.
- Hormonal and age-related factors: It is more common in post-menopausal women so there might be age and hormone factors.
- Photosensitising products: Some fragrances, essential oils and certain cosmetic or skincare ingredients may trigger this condition in susceptible patients.
Difference Between Poikiloderma of Civatte vs Melasma
An experienced clinician is usually able diagnose Poikiloderma of Civatte from its location, colour mix and distribution. However, Poikiloderma of Civatte can resemble other skin disorders like melasma, post-inflammatory hyperpigmentation and erythromelanosis. In fact, it is most commonly mistaken for melasma because both can create persistent brown discolouration on sun-exposed skin and are more common in women. However, they are not the same. Melasma is primarily a hyperpigmentation disorder, whereas Poikiloderma of Civatte usually combines pigment with redness and visible superficial vessels. The typical neck distribution and sparing under the chin also favour Poikiloderma of Civatte. Distinguishing between both these conditions matters because treatments that only target pigment may underperform when the vascular component is ignored.
How to Treat Poikiloderma of Civatte
Because this condition involves both pigment and vascular changes, there is obviously no single cream or treatment that reliably erases it. As such, a combined approach is usually necessary. Severity also dictates how much treatment is needed and how effective it can be. That’s why, it’s important to be realistic about what can be achieved and the effort needed. In general, below are some of the most effective treatments for Poikiloderma of Civatte:
- Daily sun protection: This is the foundation of management. Without strict photoprotection, improvement is harder to achieve and recurrence is more likely. Broad-spectrum sunscreen, protective clothing and limiting repeated UV exposure to the skin are essential.
- Topical depigmenting agents: Creams containing ingredients like hydroquinone or arbutin can help fade the brown pigment component in some patients. However, they do not address telangiectasia and therefore rarely solve the whole problem on their own.
- Retinoids and supportive skincare: Retinoids like tretinoin and ingredients like azelaic acid can help address broader photodamage and improve skin turnover.
- Intense pulsed light (IPL): IPL is commonly used for poikiloderma of Civatte because it can target both superficial pigment and haemoglobin-related redness.
- Vascular or pigment-targeting lasers: Lasers can be effective for targeting hyperpigmentation, redness and visible blood vessels.
Most people will require a combination of treatments for best outcomes. However, even with appropriate treatments, improvement is usually slow and gradual. Topical products, if used, need time and consistency, while IPL or laser treatments typically involve a course of multiple sessions a few weeks apart. Maintenance also matters in particular using strict sun protection and avoiding any triggers.
Can You Prevent it?
You cannot completely control intrinsic ageing or your genetic susceptibility to Poikiloderma of Civatte, but you can reduce the risk of progression. Some of the key measures that can help prevent or limit progression of Poikiloderma of Civatte include:
- Use sunscreen daily: It’s vital to use a broad spectrum sunscreen with at least SPF 30 as part of your daily routine regardless of teh weather. You should also reapply it during the day. Ensure you extend all photoprotection to the chest and sides of the neck as these areas are often forgotten and accumulate damage quietly over time.
- Be cautious with fragranced or leave-on beauty products: To reduce the risk of photosensitivity or irritation which can trigger this condition is some people, it is important to be mindful about what you put on your skin.
- Address early changes propmtly: Mild redness and hyperpigmentation are usually easier to treat than long-established severe changes.
Poikiloderma of Civatte is a common, harmless but often stubborn sign of chronic sun damage. It causes a mixed pattern of redness, hyperpigmentation and visible vessels usually on the neck and cheeks. The main reason it can be frustrating to treat is that it is not purely a pigment problem. In mild cases, sun protection and supportive skincare may help limit progression. However, more established cases often need light or laser treatment for cosmetic improvement. It is worth seeking medical assessment if you notice any skin changes especially if there is asymmetry, itch or scaling. This is because the diagnosis may not simply be Poikiloderma of Civatte. Even if it is, they will help find the best treatment path for you.
At City Skin Clinic, we strongly believe that skincare is personal and should always centre around your needs. Our doctors provide custom topical skin treatments for melasma and hyperpigmentation using ingredients like tretinoin, hydroquinone, azelaic acid, tranexamic acid and niacinamide where appropriate. If you would like a personalised skincare treatment please use our online skin consultation form or book a video consultation. Start your treatment journey today and take your first step towards great skin.
This article is intended for general informational purposes only and is not a substitute for medical advice, diagnosis or treatment. Always consult a qualified medical provider for any medical concerns or questions you might have.